The effect of hyperviscosity due to osmotic diuresis combined with alterations in the clotting cascaded caused by DKA and its treatment resulted in the formation of a large aortic arch clot in an individual who was already at risk. His preliminary hypercoaguability work up revealed a positive lupus anticoagulant, without any consequences to date. He had no personal or family history of DVT or abnormal clotting and his coagulation profile was normal on admission. Our patient was a middle aged male that had been previously healthy. Most reported cases have been associated with atherosclerotic plaque with superimposed thrombus formation and are usually detected following cerebral, visceral or peripheral embolization (2). Thoracic aortic mobile mural thrombus (TAMT) is a rare condition that is usually seen in elderly patients with extensive atherosclerotic disease, trauma or a hypercoaguable state.
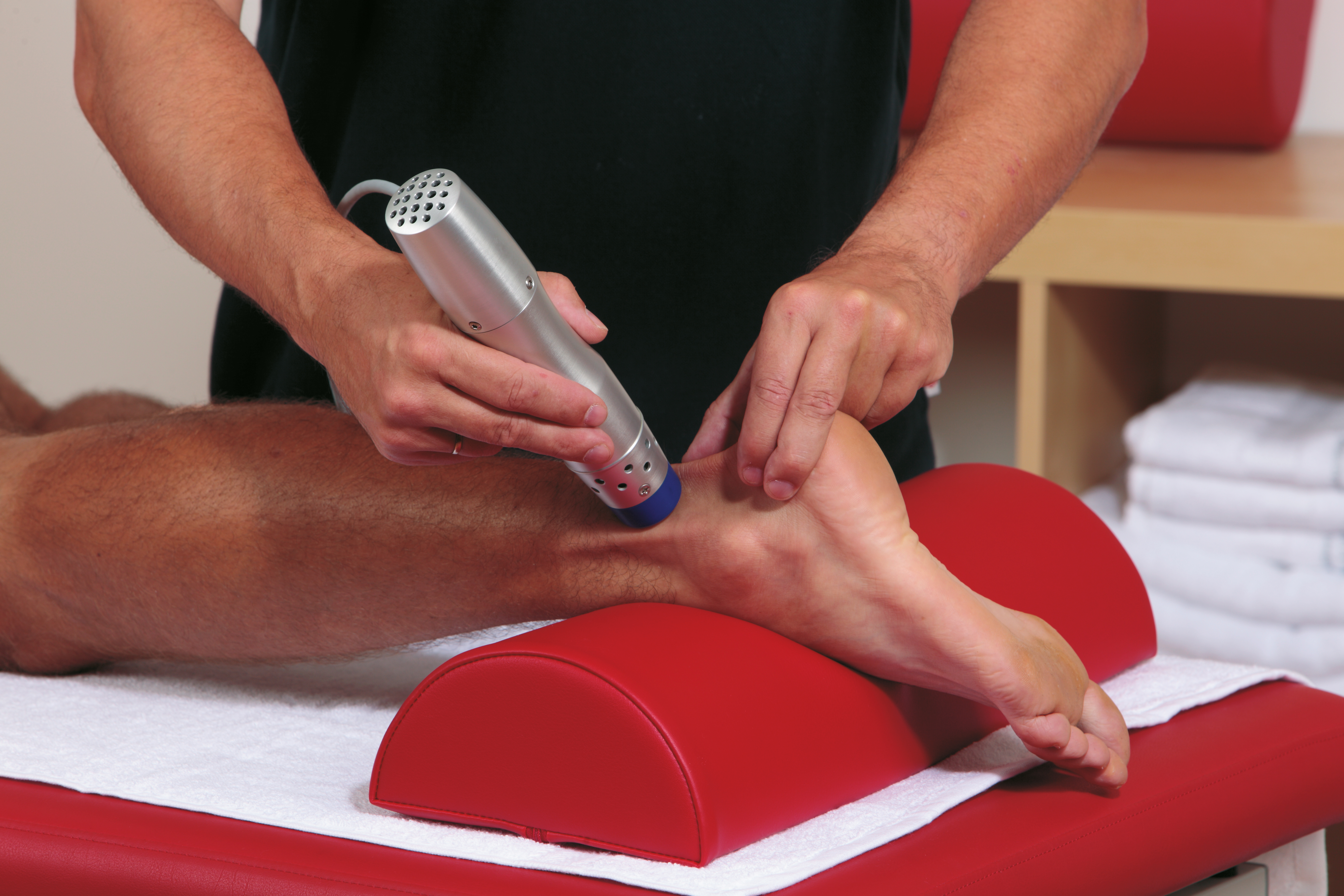
#Radial pulse free
The risks of thrombus formation are increased by treatment of DKA are thought to be due to a relative deficiency of free protein C and protein S and a relative increase in von Willebrand Factor (vWF) which in turn activates vascular endothelium (1). The pathological reports was consistent arotic thrombus.ĭISCUSSIONS: Diabetic ketoacidosis (DKA) has been shown to be a prothombotic state. The patient's lupus anticoagulant was positive. Preliminary hypercoaguability work up was sent prior to administration of heparin. Ten days later the patient was discharged home. On the following day thrombectomy was performed. He was anticoagulated with heparin and was transferred to cardiothoracic surgery service. Additionally there were smaller filling defects found in the left axillary artery. A CT aortogram showed a large filling defect in the distal ascending aorta extending into the aortic arch along its inferior wall without definite evidence of an intimal flap or pulmonary emboli. A stat bedside echocardiogram showed a mobile mass most likely representing a thrombus present at the transition from the transverse to descending aorta. The remainder of the exam was unchanged from admission. Blood pressures taken from the lower extremities were found to be 130's/80's. On exam he was found to have cool upper extremities with absent radial pulses bilaterally but normal carotid and lower extremity pulses. The patient was found awake, alert, in no distress and without new complaints. Just prior to transfer the nurse reports BP of 40/17 mmHg and informs the house-staff. On hospital day two the patient was symptomatically improved, and his DKA resolved. The patient was admitted to the MICU with new onset diabetes and DKA. 3 The radial artery can be less easily felt as it crosses the anatomical snuff box. CASE PRESENTATION: A 53 year Afro-Caribbean man with no significant medical history presents to the emergency department with a chief complaint of nausea, vomiting, polyurea, polydypsia and weakness for the three days prior to admission. Presence of radial pulse was thought to indicate a systolic blood pressure of at least 70 mmHg, as estimated from the 50 percentile, although this was found to generally be an overestimation of a patients true blood pressure.
